An Elusive Macular Hole Closed By Eye Drops Alone

A 64-year-old man presented with a 1-month history of blurred vision in his right eye (OD). His medical and ocular histories were unremarkable. On exam of his right eye and left eye (OS), VA was 20/40 and 20/20, respectively. Borderline high IOPs, mild nuclear sclerosis, and otherwise normal anterior segments were noted.
His fundus exam revealed macular edema OD; it was normal OS. Spectralis OCT (Heidelberg Engineering) high-speed 25-raster macular scans through, above, and below the fovea OD revealed macular edema and subretinal fluid (Figure 1). As the appearance was suggestive of a macular hole (MH), a high-density OCT scan was performed, revealing a small MH missed during the standard OCT scan (Figure 2).
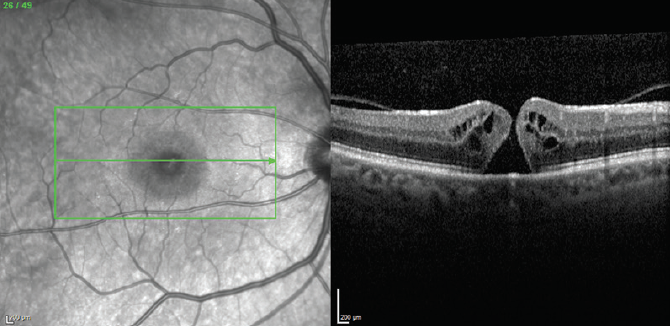
Figure 2. High-density OCT scan through the fovea demonstrating a small MH.
THERAPY AND RESULT
Given the small size of the MH and presence of edema at its edges, medical treatment with a topical NSAID was offered as an alternative to surgery.
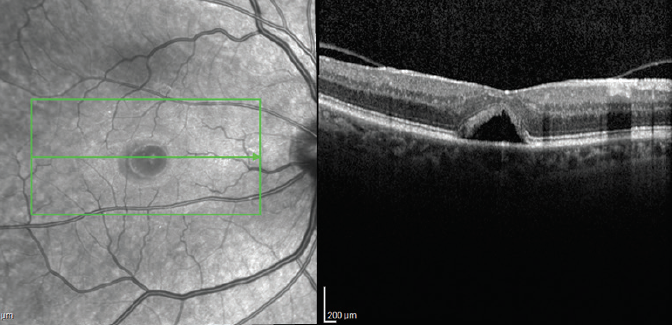
Figure 3. High-density OCT scan through the fovea 6 weeks after starting NSAID treatment showing a closed MH with subfoveal fluid pocket.
The patient was prescribed ketorolac eye drops 0.5% three times a day OD. After 6 weeks, the MH closed and a small pocket of subfoveal fluid persisted, but no macular edema was noted. The patient’s visual acuity and symptoms had not changed (Figure 3).
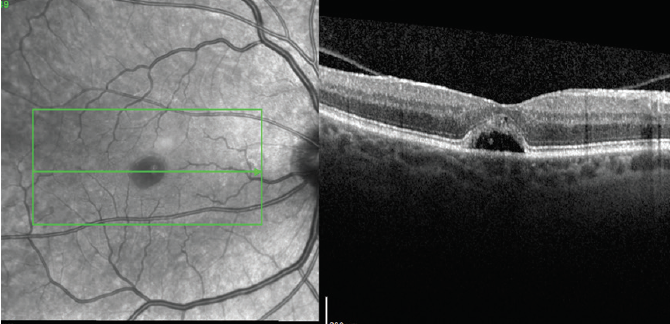
Figure 4. High-density OCT scan through the fovea 4 months after starting treatment showing a closed MH with a slightly smaller subfoveal fluid pocket.
Over the next 4 months, the drops were gradually tapered. At the patient’s last visit, at which point he was using ketorolac once daily, the MH remained closed with reduced subfoveal fluid and unchanged visual acuity or symptoms (Figure 4).
COMMENTARY
MHs are believed to form due to tractional forces at the vitreoretinal interface. In 2003, Tornambe proposed a hydration theory of MH formation,1 whereby posterior hyaloid traction creates a small inner foveal retinal defect which then absorbs vitreous cavity fluid, causing retinal swelling around the defect. As the inner retina swells, it retracts anteriorly, widening the hole.
This theory suggests that reversing the hydration process may lead to hole closure. Surgery with internal limiting membrane peeling and gas bubble tamponade accomplishes this with a high degree of success.
It stands to reason that, if the retinal hydration can be reduced medically, the MH should close without surgery, which it did in the case presented here. The hole closed, and likely over time the subfoveal fluid pocket will reabsorb. In an analysis of OCT findings in surgically closed MHs in the PIONEER study, subfoveal fluid was present in 49% of eyes at 1 month after surgery, decreasing to 37% at 6 months.2
In the case presented here, the subfoveal fluid was improving at the patient’s most recent visit, similar to what is seen in surgically closed MHs, but it may take a year or longer to fully resolve.
Our choice of ketorolac was based on insurance formulary coverage and the cost to the patient. Any of the available NSAID drops would be suitable for a similar patient.
LESSONS TO LEARN
Although prospective randomized clinical trials are the gold standard for validating treatments, new treatment modalities can be introduced to the retina community based on anecdotal experience shared with others.
Two lessons can be drawn from this case. First, standard OCT scans can miss a small MH. If there is a high degree of clinical suspicion that an MH is present based on other clinical features, a high-density scan through the fovea may reveal the hole.
Second, for small MHs with some degree of retinal edema, a trial of NSAID drops is a reasonable initial treatment option, avoiding the potential adverse effects and patient inconvenience of surgical treatment without compromising future surgical treatment if needed.
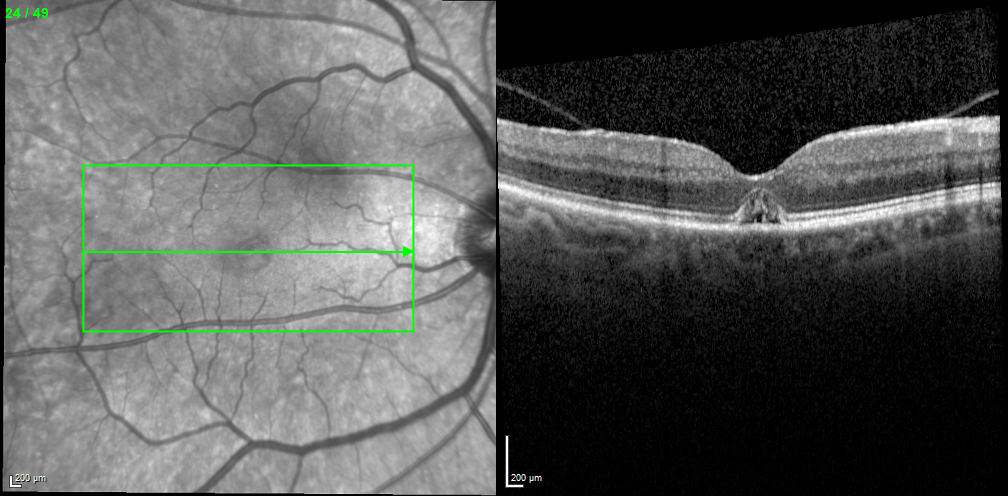
UPDATE ON THE CASE
After this article went to press, the patient returned for follow-up. As of February 2020, the patient’s VA was 20/30 and further fluid reduction had been demonstrated.
- Tornambe PE. Macular hole genesis: the hydration theory. Retina. 2003;23(3):421-424.
- Ehlers JP, Han J, Petkovsek D, Kaiser PK, Singh RP, Srivastava SK. Membrane peeling-induced retinal alterations on intraoperative OCT in vitreomacular interface disorders from the PIONEER study. Invest Ophthalmol Vis Sci. 2015;56(12):7324-7330.
Brian C. Joondeph, MD, MPS
• Partner, Colorado Retina Associates, Denver, CO
• bjoondeph@retinacolorado.com
• Financial disclosure: None
Madeleine Webb, BA, BS
• Ophthalmic Technician, Colorado Retina Associates, Denver, CO
• mwebb@retinacolorado.com
• Financial disclosure: None

